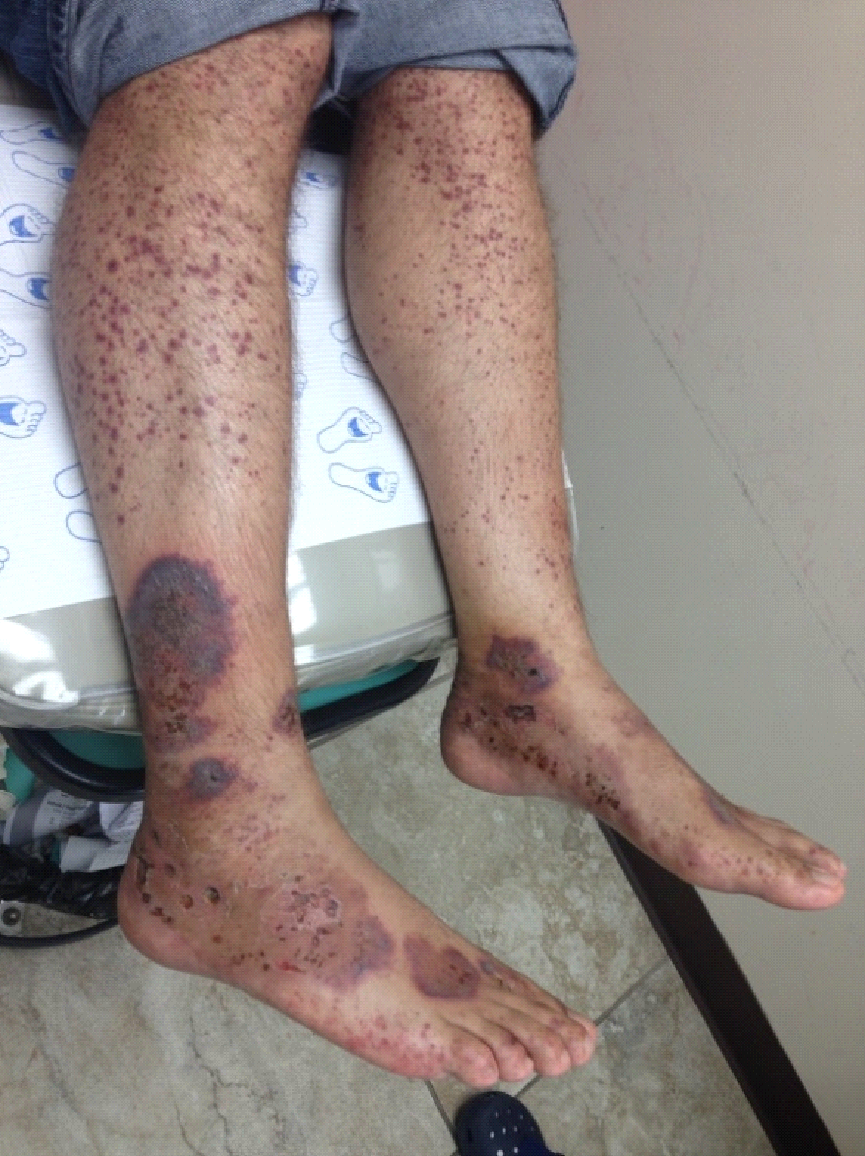
Symptoms
Superficial bleeding (petechiae, purpura, mucosal bleeding), epistaxis, menorrhagia
Etiology
| Category | Conditions |
|---|---|
| Autoimmune | ITP, SLE, RA |
| Consumption | HUS/TTP, DIC, HT |
| Production | Bone marrow failure (presents as pancytopenia), Myelodysplasia, B12/Folate deficiency |
| Drug induced | NSAIDs, sulfa drugs, IIb/Illa inhibitors, Heparin, Quinine, EtOH |
| Infection | HIV, Hep C, EBV |
| Genetic | Bernard Soulier (AR Defect in GPIb-IX), Glanzmann Thrombasthenia (AR Defect in GPIIb-Illa) |
| Sequestration | Seen with hypersplenism, portal hypertension |
| Pseudo | Pseudothrombocytopenia (platelet clumping, resulting in abnormal test) |
| Special Scenarios | Malignancy (bone marrow invasion or DIC), Pregnancy (gestational thrombocytopenia, preeclampsia, HELLP), Liver failure (I TPO, splenic sequestration) |
| Uniat Superficial bleeding | Petechiae, purpura, mucosal bleeding, epistaxis, menorrhagia |
Investigations
- Exam for signs of bleeding
- CBC in citrated blood tube, INR, PTT, fibrinogen, D-dimer, blood smear
- Additional considerations: Heparin-PF4 antibody (if 4T-score is 4-8), ultrasonography for DVT evaluation, ferritin (if concern for HLH), liver function tests (if cirrhosis suspected), TEG in complex cases
Immediate concerns
- Evaluate risk of bleeding: Review anticoagulant medications, consider discontinuation, and platelet transfusion if necessary
- Consider HIT (Heparin-Induced Thrombocytopenia)
- If schistocytes are present, consider TTP (Thrombotic Thrombocytopenic Purpura)
Treatment
- Want platelets > 50k prior to procedure
- Platelet transfusion: Active bleeding with count < 50k OR any person < 10k
Heparin Induced Thrombocytopenia
Etiology
- HIT results from autoantibodies that react to a combination of heparin and platelet factor 4 (PF4), leading to platelet activation and thrombosis
- Risk factors include female sex, older age, obesity, and hemodialysis
- Consider HIT in patients recently treated with heparin who have new-onset thrombocytopenia, skin necrosis at injection sites, anaphylactoid response to heparin, or venous/arterial thrombosis
Risk Stratification and Diagnostic Tests for HIT
- Use the 4T score for risk stratification
- The heparin-PF4 antibody test has high sensitivity but poor specificity
- Serotonin Release Assay (SRA) is the gold standard diagnostic test, but it is expensive and time-consuming
4Ts Score for Heparin-Induced Thrombocytopenia
Management and Treatment of HIT
- Initiate empiric anticoagulation therapy for HIT in patients with clinical thrombosis on therapeutic heparin anticoagulation
- Switch heparin to a non-heparin agent such as argatroban
- For patients without clinical thrombosis but a high likelihood of HIT, empiric anticoagulation with a non-heparin agent should generally be started before confirmation of the diagnosis
- Non-heparin anticoagulants
- Argatroban is perhaps most commonly used (with a similar option being Bivalirudin)
- Fondaparinux could be considered in intermediate-likelihood situations, at a reduced dose (2.5 mg sq daily)
